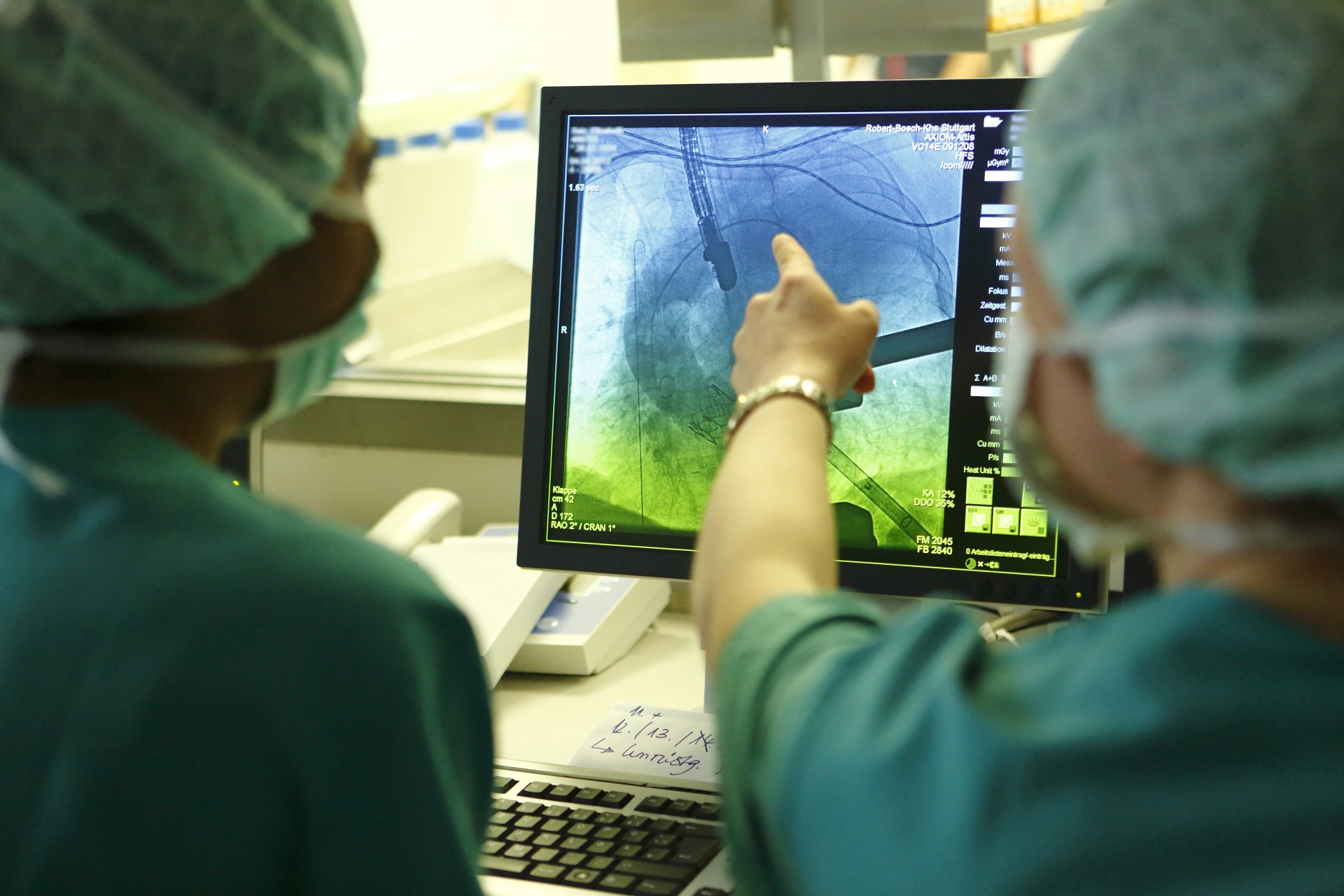
“We risk the teslaization of medicine in Germany”
The advantages digitalization brings to health care are as obvious as the damage any further delay will cause. But there are grounds for hope.
The German health care system certainly proved its worth during the pandemic. While it was, in some cases, pushed to its limits, with staff working far beyond what was reasonable, on the whole the system withstood the test. That said, I am convinced that our health care system can only survive at its current level if we systematically forge ahead with digitalization.
The need is clear. We are still right in the midst of the pandemic and the numbers the Robert Koch Institute (Germany's national Public Health Institute) reports every single day are still high. But at the same time, we know frighteningly little about how the pandemic actually looks across the country. We don’t know how many people are currently in hospital, nor do we have any precise data on who has been vaccinated. Why? Because vaccinations are still recorded in little yellow booklets with no digital record made. As a result, we have no way of making any truly sound statements on the vaccine’s efficacy. We find ourselves in this absurd reality where one of the vaccines was co-developed here in Germany, but we are forced to gather all our information about it from abroad – from Israel, for instance.
“We find ourselves in this absurd reality where one of the vaccines was co-developed here in Germany, but we are forced to gather all our information about it from abroad.”
Efficient, smart, and rapid data handling is more urgent than perhaps ever before, and this can only be digital. The days of fax machines and yellow vaccination cards are without a doubt over. But stopping the spread of the pandemic is by no means the only point at which the urgent need for digitalization is glaringly obvious. I believe this is the only way to effectively counter demographic change with a well-functioning health care system.
Today, family physician care is already no longer a given in many places, a development sure to have a dramatic impact on a country with a rapidly aging population. At the same time, however, the disruptive potential digitalization holds is becoming clear. A smartwatch is already capable of collecting a whole host of relevant health data. Simply by pressing it with my finger, I can produce an ECG or get a certified diagnosis of whether I have atrial fibrillation – all in just 30 seconds. Nowadays, you can have three professionals all on your wrist: doctor, nurse, and administrator. The smart transmission of relevant health data could potentially replace many a visit to the family doctor or specialist and even inpatient stays in as little as five years.
“The disruptive potential digitalization holds is becoming clear.”
In addition, an enormous range of possibilities is opening up when it comes to monitoring the health of older people or those otherwise in need of assistance. Not only does this improve efficiency, in sparsely populated regions it can even ensure basic medical care, with tangible benefits for patients. Older people usually want nothing more than to remain in a familiar, home environment. Smart digital solutions can make this a reality.
On the other hand, the German health care system is currently still characterized by a major chasm between outpatient and inpatient care. The right sensor technology is one way to close this gap and, in an ideal world, establish a stable continuum of treatment. Doctors would be able to predict early on when hospital-based clinical intervention is needed.
For patients, however, digitally documenting all relevant data would have a second key advantage: It would be easy to draw together any information relevant to treatment and access it via a smartphone, for instance. This applies when checking into a hospital, but also when switching from one specialist treatment to the next – all relevant data would be available instantly, as is already the case in Israel and to a certain degree in the US. Patients would be the owners of their own data and could obtain information relating to their results independently.
Alongside these two closely linked fields, namely patient data and smart diagnostics, health care is currently experiencing a third major digital trend: artificial intelligence and robotics. A few years down the line, artificial intelligence will be the default in helping to evaluate MRI or X-ray images. Similarly, in no time at all, it will be possible to create an overview of vast numbers of comparative cases, thus optimizing treatment. Wherever there are large amounts of digital information, artificial intelligence will play an invaluable role. But therein lies the paradox: Precisely what that needs is a large amount of data. If this data is not available in Germany, we risk what I call the teslaization of medicine, whereby Germany, a former hub for cutting-edge technology, will be left behind on an international level.
“Hesitation and procrastination have ruled the roost for too long. It’s time to act.”
But I do see light at the end of the tunnel. The new German government’s coalition agreement states that an electronic health record (ePA) will not only be introduced but will also function on an opt-out basis. This means that everyone will receive their own personal digital health record, and those who do not wish to do so will have the option to opt out. If we can then ensure that these larger data packages are run via public and legal, and thus ultimately state, institutions and are not purely commercial from the outset, I expect they will meet with widespread approval among the population.
If I could ask for anything from the German health care system, it would be for there to be the political will to push ahead with digitalization. This includes making the necessary financial resources available. And lastly, it is vital to engage in dialogue with the general public on the topic at an early stage. Hesitation and procrastination have ruled the roost for too long. It’s time to act.